Runny Nose — Causes, Quick Fixes, and When to See a Doctor
A runny nose is annoying, but usually not dangerous. It can mean a simple cold, seasonal allergies, or a reaction to smoke, perfume, or a change in weather. This page gives practical tips you can use right away, plus clear signs that mean you should get medical help.
Common causes you can spot at home
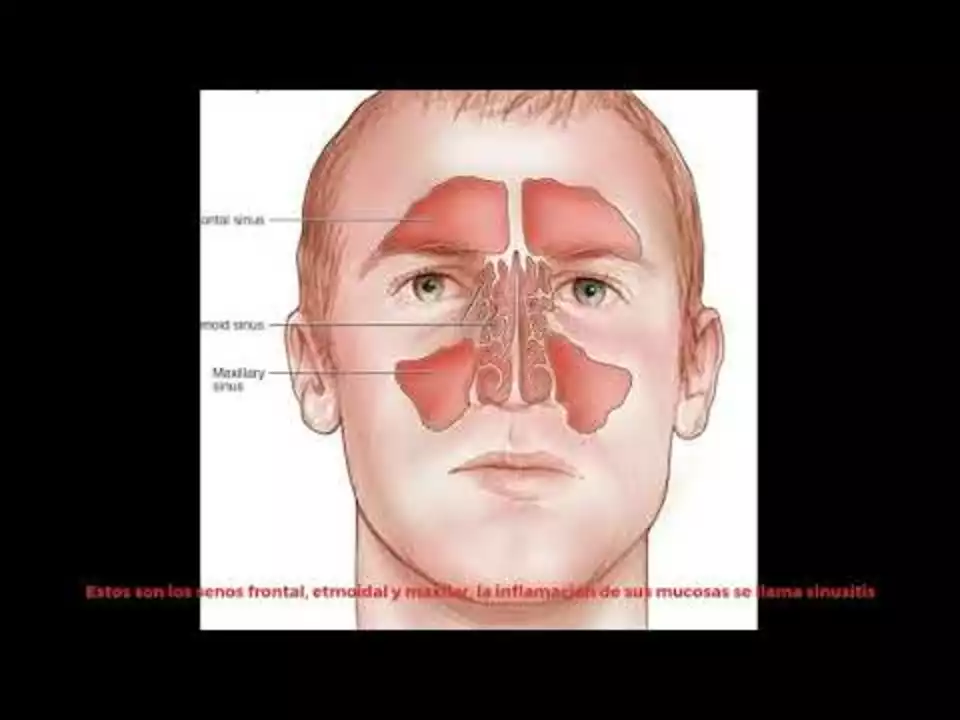
Viral colds are the top cause — expect clear watery mucus, sneezing, sore throat, and mild fatigue for a few days. Allergies (hay fever) usually bring itchiness in the eyes and nose, watery clear discharge, and symptoms that repeat around the same time each year or when you meet pets or dust. Sinus infections often start like a cold but switch to thicker yellow or green mucus, face pressure, and tooth pain. Irritants like smoke, cold air, or strong smells can trigger a temporary runny nose too.
Quick relief and home care that actually helps
Saline nasal spray is safe and effective — use it 2–4 times a day to flush mucus and allergens. A humidifier at 40–50% helps thin secretions and stops your nose from drying out. Steam from a hot shower or a bowl of hot water for 5–10 minutes can loosen mucus quickly. For babies, a few saline drops and a bulb syringe make breathing easier.
Over-the-counter options: second‑generation antihistamines like cetirizine or loratadine work well for allergy-related runny nose and won’t make you drowsy. First‑generation antihistamines such as diphenhydramine reduce drip but often cause sleepiness. Oral decongestants (pseudoephedrine) can clear nasal congestion but avoid them if you have high blood pressure or heart disease. Topical nasal decongestant sprays (oxymetazoline) give quick relief but use for no more than 3 days to avoid rebound congestion. Nasal steroid sprays (fluticasone, budesonide) are best when allergies are the cause — they take a few days to reach full effect, so use daily.
Try padding your pillow, staying hydrated, and avoiding known triggers like smoke or strong scents. If mucus is thick, warm compresses over your sinuses and gentle nasal irrigation (neti pot with sterile or boiled-and-cooled water) can help.
When to see a doctor: if symptoms last more than 10 days without improvement, you have a high fever (over 101°F / 38.3°C) or worsening face pain, green or bloody nasal discharge with fever, breathing trouble, wheezing, or severe ear pain. Babies under 3 months with fever or any infant who seems very ill should see a doctor right away. If you think it might be COVID-19 or you’re high risk, test and contact your provider.
If you’re unsure whether it’s allergies, a cold, or a sinus infection, your clinician can quickly sort it out and suggest the right treatment — sometimes a short antibiotic for a clear bacterial sinus infection or a prescription nasal spray for bad allergies. Simple fixes often work, but don’t wait if symptoms get worse or stick around.