Gastrointestinal symptoms: common causes and what to do
Stomach pain, bloating, diarrhea or heartburn can ruin your day — and they often mean different things. Knowing quick steps to feel better and the signs that mean you need medical help makes a big difference.
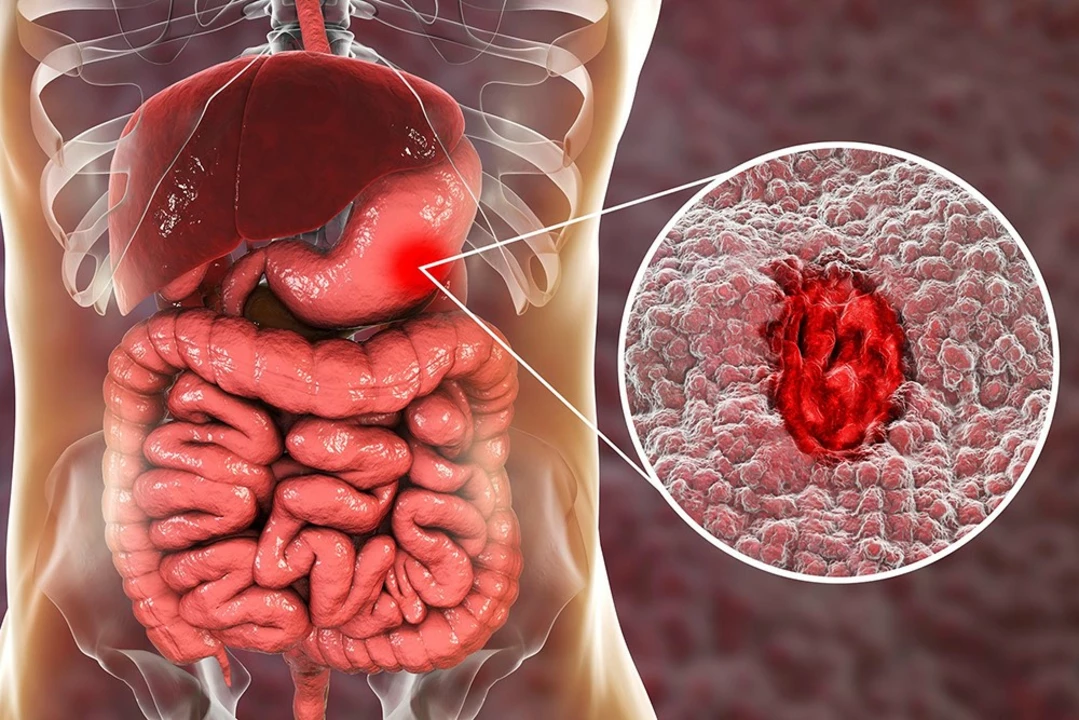
Common causes include food choices like spicy or greasy meals, lactose or other intolerances, viral stomach bugs, side effects from medicines such as antibiotics or NSAIDs, and acid reflux. Stress and functional disorders such as irritable bowel syndrome can trigger long‑running symptoms without visible damage. Less common causes that need testing are ulcers, gallstones, pancreatitis, infections, and inflammatory bowel disease.
When to see a doctor
If you spot any of these, get medical care fast: severe or worsening abdominal pain, vomiting that won’t stop, fever with belly pain, bloody or black stools, unexplained weight loss, or signs of dehydration like fainting or very little urine. Also see a doctor if symptoms last longer than two weeks or keep coming back. If you take prescription drugs for the heart, blood pressure, or cancer, check with your provider before using over‑the‑counter remedies for stomach issues.
Simple home steps that help
Start with hydration. Sip water, oral rehydration solutions, or clear broths if you have diarrhea or vomiting. Eat small bland meals — toast, bananas, rice, applesauce — until your stomach calms down. Avoid alcohol, caffeine, fatty foods and heavy spices for a few days. For heartburn, antacids or H2 blockers can give fast relief; if you use multiple meds, especially blood thinners or heart drugs, run those choices by a pharmacist or doctor first.
Watch how medicines affect your gut. Antibiotics can cause diarrhea or yeast overgrowth, and NSAIDs can irritate the stomach lining. If a medication seems to trigger symptoms, don’t stop it without talking to your prescriber. Sometimes switching to a safer alternative or adjusting the dose fixes the problem.
Practical tips for ongoing issues: keep a food and symptom diary to spot triggers, try smaller more frequent meals, and reduce stress with short walks or breathing breaks. If you have chronic reflux, ask your doctor about long‑term options beyond antacids, including lifestyle changes or prescription medicines.
Our site has guides that dig deeper into related topics like alternatives for acid reflux meds, antibiotic side effects, and safe online options for blood pressure drugs. Use trustworthy resources and avoid random forums for medical advice.
If you’re unsure what’s causing your symptoms, a primary care visit often sorts it out. Tests like bloodwork, stool checks, breath tests for intolerances, or imaging can identify infections, inflammations, or structural problems. Getting the right answer early lets you pick the right treatment and feel better faster.
Keep a clear list of all medicines and supplements to show your clinician — interactions or recent changes often explain new stomach problems. If travel or new food rules are involved, mention that. For sudden severe symptoms, emergency care is safer than waiting. Early action often avoids hospital visits. You can start today now.